The Culturally Responsive Intersectional Stigma Prevention Intervention
PARTICIPATING
Healthcare Facilities
PROSPECTIVE
Healthcare Facilities
Black men who have sex with men (MSM) face a unique intersection of stigmas related to race, sexuality, gender expression, and HIV risk, and these stigmas combine to create additional barriers to healthcare access. The Culturally Responsive Intersectional Stigma Prevention (CRISP) intervention is a package of training, skills building, technical assistance, and quality improvement activities aimed to increase providers’ awareness of these stigmas and to reduce health disparities through developing skills responsive to the specific needs of Black MSM .
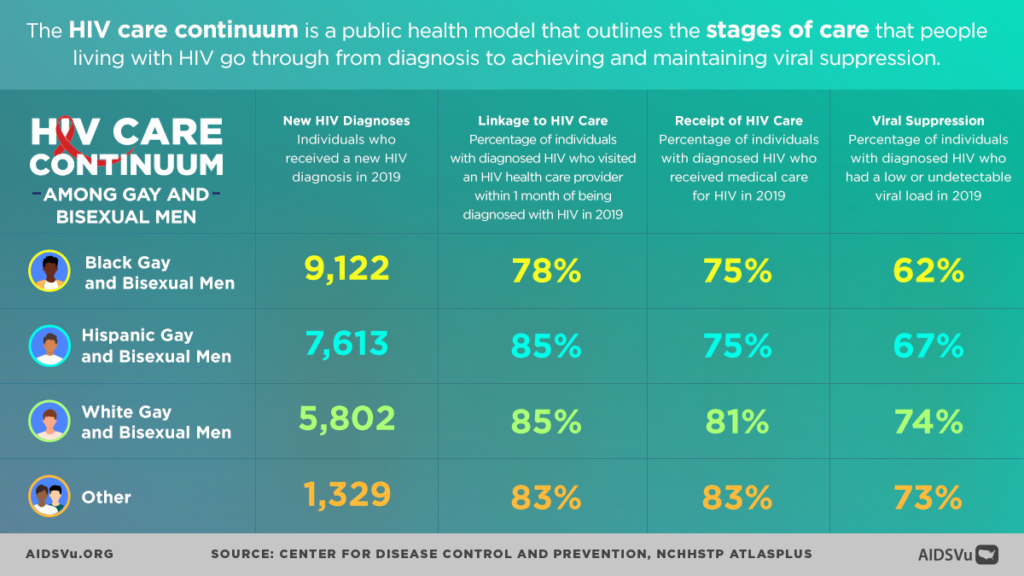
Healthcare for Black MSM must be optimized across the entire HIV continuum, from testing to prevention to treatment.
WHY IS STIGMA PREVENTION IMPORTANT?
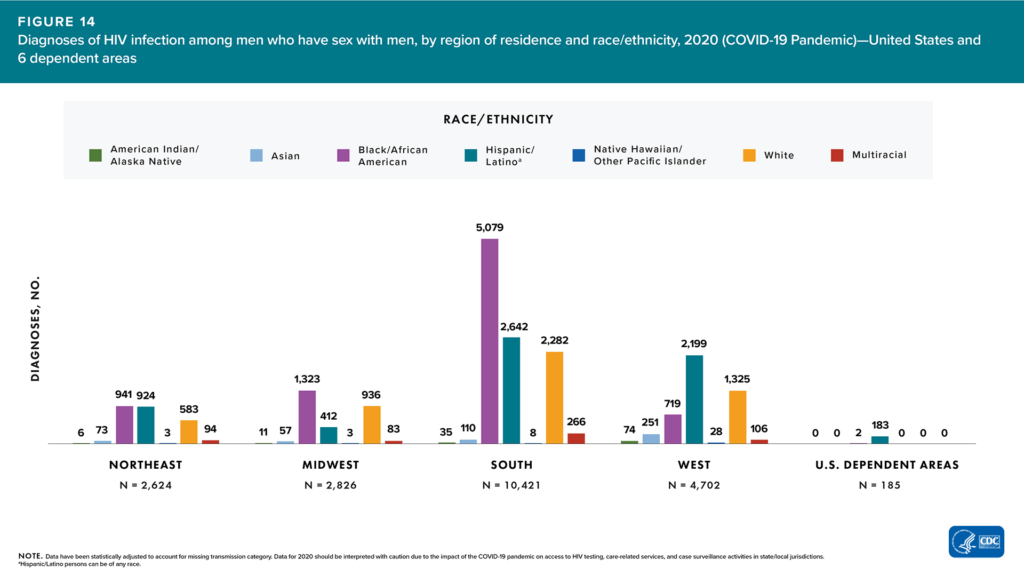
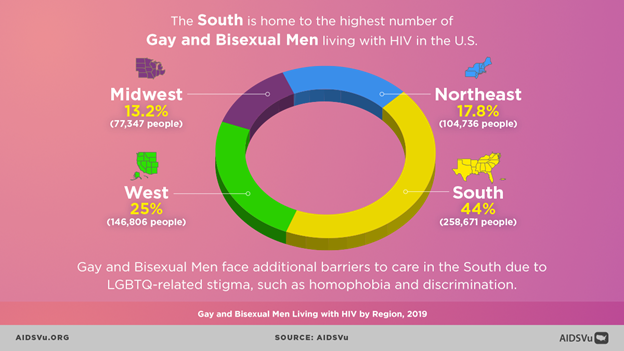
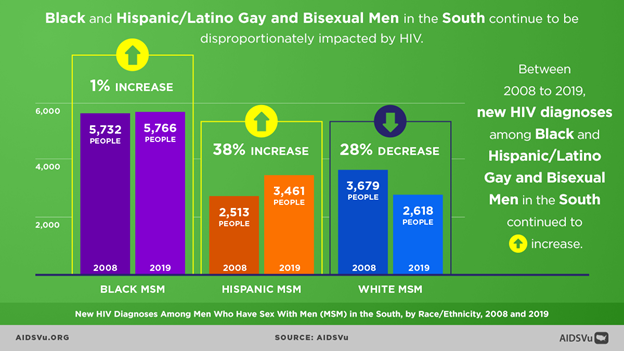
The US HIV epidemic is concentrated in the South. Among MSM in the South, Black MSM make up almost half of the new infections. Despite biomedical advances, inequities persist in the utilization of HIV prevention and care services by Black MSM, particularly in the South. HIV biomedical prevention and treatment interventions have not had the same impact for Black MSM as they have for other groups.
Interventions to increase the use of biomedical prevention and treatment are imperative, but will only occur if health settings and providers are culturally responsive to Black MSM needs.
The healthcare environment is key to either facilitating – or impeding – Black MSM engaging with testing, PrEP, or HIV treatment.
i.e. White people represent 65% of PrEP users while accounting for 26% of new HIV diagnoses, while Black people represent only 14% of PrEP users while accounting for 42% of new HIV diagnoses, indicating a large disparity in access and care.
Many Black MSM have had negative experiences in health care settings resulting in a feeling of judgment, rejection, shame and guilt, and ultimately medical mistrust. Negative interactions with healthcare staff discourage HIV testing and disrupt linkage to care, and the perception of stigma can cause Black MSM to avoid healthcare services due to fear of being discovered or identified, and/or fear of discriminatory treatment.
Intensive, skills-based training and quality improvement methodologies are proven means of reducing stigma at healthcare facilities. CRISP is designed to help healthcare facilities demonstrate cultural responsiveness when providing services to Black MSM.
HOW DOES CRISP WORK?
CRISP is comprised of a bundle of six integrated components that are implemented at healthcare facilities over a two-year period. Implementation of the CRISP program is designed to be adaptive and flexible, taking into consideration busy clinic schedules and multiple competing priorities.
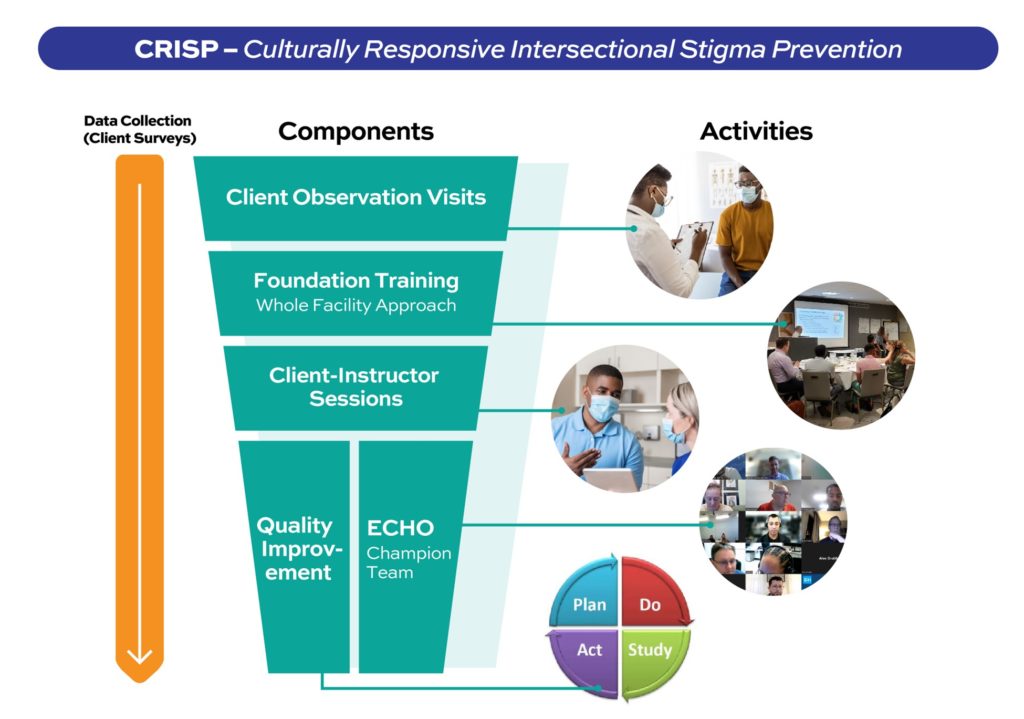
Client Observation Visits
Also called Simulated Assessment Visits (SAVs), one of the first CRISP activities trained Black MSM “Client Instructors” will visit each clinic and complete simulated visits (“test patients”) to assess their general experience of the healthcare facility from the perspective of a Black MSM client. The Client Instructors will provide qualitative feedback to each clinic to inform later quality improvement activities.
Foundation Training
The CRISP intervention starts with a foundational 2-day workshop that aims to enhance cultural responsiveness in providing HIV care and prevention services for Black MSM through greater awareness and understanding of how anti-Black racism and other intersectional stigmas affect their HIV and sexual health behaviors, in order to improve their health outcomes along the HIV continuum. This interactive, skills-based workshop focuses on communication skills that support Black MSM in HIV PrEP and treatment linkage, retention, re-engagement, and adherence, and identifies structural interventions to increase cultural responsiveness in clinical settings and services.
Client-Instructor Coaching Sessions
Trained Black MSM “Client-Instructors” will hold one-on-one coaching sessions with providers after the Foundation training to provide an opportunity and safe space for providers to practice interpersonal communication skills around PrEP or ART initiation with Black MSM clients. Providers will complete a simulated patient interaction with the Client-Instructor and then receive coaching and feedback on specific competencies.
Quality Improvement Learning Network
A guided quality improvement approach is taken to implement small tests of change and self-monitor improvement data over time, bolstered by ongoing facilitated peer-to-peer learning. Each site is paired with a quality improvement coach and will be part of a peer learning network to help foster ideas and provide guidance throughout the QI process.
ECHO Case-Based Learning
With a smaller subset of staff (referred to as a Champion team), additional training sessions are held virtually focusing on a variety of topics to explore more deeply after the Foundation training. Each session includes a short didactic and then a case-based peer knowledge exchange related to the session theme.
Client Climate Surveys
Clients of the healthcare facilities will be asked to complete periodic surveys assessing the healthcare environment to see how experience of the clinic may change over time. Summary survey results by patient demographic will be provided to each clinic to inform their quality improvement approach.
WANT TO GET INVOLVED?
Participating facilities must be located in an intervention community. Within this community, any healthcare facility that provides HIV testing, HIV PrEP/prevention, and/or HIV treatment and care services to Black men would be eligible. This may include, but is not limited to:
Examples of eligible facilities:
- HIV treatment clinics/providers (public and private)
- Primary Care Providers (providing PrEP)
- Community health centers and FQHCs
- CBO-based health services including AIDS Service Organizations
- Public health and health department clinics, including STI testing and treatment centers
- Hospital outpatient clinics
- College/university health services
- Retail health hubs/pharmacies
BENEFITS OF PARTICIPATING
TRAINING FOR CLINIC STAFF
With an inclusive whole facility approach and one-on-one client-instructor skills application and mentoring.
FACILITATED QUALITY IMPROVEMENT PROGRAM
Featuring guided self-monitoring of clinical, patient, and health worker data; rapid improvement cycles; coaching and technical assistance; and peer-to-peer learning.
PEER LEARNING NETWORK AND KNOWLEDGE EXCHANGE
CLIENT SURVEY FEEDBACK
Participating facilities will receive a small annual compensation package intended to offset any revenue loss or staff resource burden as a result of participating in CRISP activities. The compensation is a flat fee and not intended to reimburse salary or staff time directly, but to acknowledge the investment that facilities are putting into this program and provide some additional resources to them. These funds are unrestricted but will be tied to reaching milestones in the CRISP program.
Ultimately, the intended outcome of the program is improved service delivery and quality outcomes for Black MSM at your facility, which will contribute to reaching EHE goals in your community.
Interested?
Contact us below if you’d like to get involved or have any questions.